Summary :
◉ What is Hidradenitis suppurativa ?
Hidradenitis suppurativa is a chronic, painful, non-contagious inflammatory skin disease that causes painful bumps under the skin in the hair roots near certain sweat glands.
The exact cause is unknown, it takes many forms (acne, boils, etc.) and it develops in areas of frequent compression and friction of the skin such as the armpits, groin, buttocks and boobs.
There is no cure for Hidradenitis suppurativa, but treatments and lifestyle changes can provide some relief and reduce flare-ups.
Other names for the disease are hidradenitis, Verneuil's disease or inverted acne.
Hidradenitis suppurativa was first described by Velpeau (1839) but Verneuil (1854) recognized it to be a disorder of the apocrine sweat glands.
◉ Causes
Verneuil's disease develops when hair follicles become clogged. The exact cause of this is not known. Experts believe it could be related to hormones, genetic predisposition, smoking or being overweight.
It is not caused by infection or soiling, and it cannot be transmitted to other people.
◉ Hidradenitis suppurativa risk factors
Factors that increase your risk of developing Hidradenitis suppurativa include:
- Age : The risk of Hidradenitis suppurativa is highest in people in their 20s and 30s. It is more rare after 50 years
- Gender : Women are more likely to develop Verneuil's disease (3 women / 1 man), although men generally have more severe symptoms.
- Ethnicity : The prevalence of the disease is disproportionately high among black people.
- Family history : 30 to 40% of patients have at least one affected family member.
- Smoking : Smoking increases risk and worsens symptoms.
- Obesity
- Diabetes, hypertension, hypercholesterolemia, etc.
- Stress
- Too tight clothes
◉ Hidradenitis suppurativa symptoms
Early symptoms of Hidradenitis suppurativa can range from mild itching and discomfort to red, tender, swollen areas or a painful inflamed bump.
The lesions generally affect both sides of the body, they are limited to a single place or to several areas at the same time.
Verneuil's disease is divided into three stages, depending on its severity, called Hurley stages:
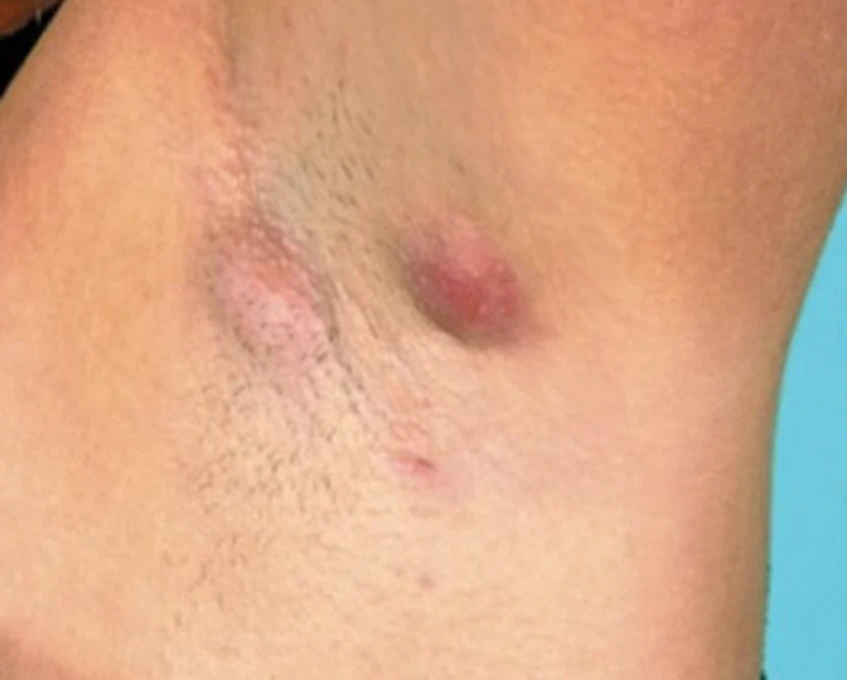
- Stage 1: Usually presents as an inflammatory nodule or abscess, single or multiple, without sinus tracts or scars.
- Stage 2: Usually presents as abscesses and nodules, isolated or multiple, widely separated, with sinusitis formation or scarring (rope-like elevation of the skin).
- Stage 3: Usually presents as diffuse or near-diffuse involvement with multiple interconnected sinus pathways, scarring, and abscesses over the entire surface
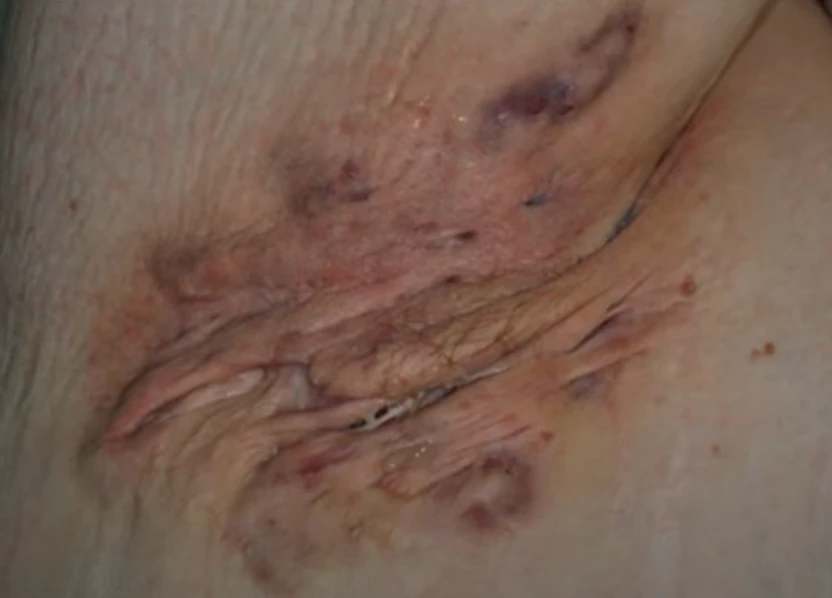
Hidradenitis suppurativa stage 3
Lesions usually occur in areas where you have hair or where your skin rubs together, such as :
- Under the arms
- The groin
- Between the buttocks
- Between the thighs
- Under the breasts
- In the folds of the belly
- On the neck
- Behind the ears
Note :
- Misdiagnosis is common, with early lesions of Verneuil's disease often mimicking other diseases.
- The course of the disease is highly variable
◉ Diseases associated with Verneuil's disease
People with Hidradenitis suppurativa often have other medical problems:
- Acne conglobata: nodulo-cystic acne.
- Heart disease
- Dissecting cellulitis
- Crohn's disease
- Polycystic ovary syndrome
◉ Diagnosis
The diagnosis is essentially clinical, no biological or pathological examination is necessary, in particular in well-developed lesions.
Clinical diagnosis requires recognition of morphology, location (intertriginous areas, areas containing apocrine glands) and chronicity of the disease process (prolonged course with periods of activity and remission).
The doctor will ask questions and do a physical exam:
- Look for a family history of skin problems.
- Research a personal history of skin problems.
- Lesion history: typically, recurrent lesions more than 2 times in 6 months.
- Perform a complete skin examination: multiple deep inflamed nodules, gravel comedones, sinus tracts, abscesses and/or fibrotic scars
Note
- A biopsy is beneficial in cases where the diagnosis is uncertain or to exclude squamous cell carcinoma.
- Ultrasound may be useful for preoperative assessment.
- Bacterial cultures may be requested if a secondary infection is suspected
◉ Differential diagnosis
- Acne vulgaris
- Follicular pyoderma (folliculitis, boils, carbuncles)
- Intergluteal pilonidal disease
- Crohn's disease
- Inguinal granuloma
- Tuberculous abscess
- Nodulo-ulcerative syphilis
◉ Treatment
There is no cure for hidradenitis. Drug treatment, surgery, or both can help control symptoms and prevent complications.